Dr Benjamin Dummer is a Research Assistant based in a lab at the University Hospital of Wales (UHW), under the supervision of Professor Liam Gray.
The research
Our current research focuses on glioblastoma, which is a deadly brain cancer. We are characterising a 3D cell culture model using brain tumour tissue direct from surgery. This will allow us to personalise medicines to individual patients and gain a better understanding of glioblastoma biology.
We are also collaborating with other research groups within Cardiff University and outside institutions to explore how our 3D model can be used to better understand other neurological diseases.
Despite decades of research and millions of pounds spent, patient outcomes for people diagnosed with glioblastomas is still very poor. There is a clear need for developing novel treatments to combat the disease. Within these tumours there is a subpopulation of cells called stem cells which are implicated in treatment resistant and disease progression. Understanding how these cells interact with each other and their microenvironment is a fascinating area of research which will hopefully lead to a better understanding of this deadly disease.

What next?
Our next step is to complete the work on our 3D model so we can move forward to developing a personalised medicine paradigm with the aim of helping patients who suffer with this horrible disease.
BRAIN researchers have co-edited a book which examines the progress of cell therapies in the treatment of neurodegenerative diseases, published last November.
Cell therapies are a promising development for the treatment of neurodegenerative diseases (NDDs) such as Huntington’s and Parkinson’s, which occur when nerve cells in the brain or the nervous system stop working or die.
The symptoms of NDDs are varied and can range from memory loss and mood disorder to mobility issues. Existing medicines for NDDs aim to minimise some of these symptoms but are unable to treat the root causes of the disease itself.
New therapies such as Advanced Therapeutic Medicinal Products (ATMPs) are a new and personalised alternative to treating NDDs. Unlike existing medicines, ATMPs aim to treat the direct cause of disease whereby cells, protein, or DNA is extracted from a patient before they are altered and then re injected.
The BRAIN Unit, based at Cardiff University is examining the effects of ATMPs in a series of clinical trials. Clinical trials enable researchers to test the effectiveness of a new treatment and ensure it is safe enough to use on a wider scale.
The new book, ‘Current Challenges in Cell Therapy for Neurodegenerative Diseases’ is co-edited by three of BRAIN’s researchers: Emma Lane, Mariah Lelos and Cheney Drew and was commissioned as part of the International Review of Neurodegenerative Diseases. The book examines the progress of such ATMPs, as well as some of the challenges of translating these therapies into a clinical setting.
As well as editing the volume, Lane, Lelos and Drew also contributed chapters to the book, aligned with their current areas of research. This includes the development of stem cell therapies for Parkinson’s and Huntington’s disease and how those are investigated with the use of animal models, how we can evaluate ATMPs in clinical trials and the importance of including the patient voice in the development and testing of new treatments.

Cheney Drew said, “We are delighted to bring together leading international experts in the development and clinical translation of cell and gene therapies in neurodegenerative disease. The contributions to this volume cover the breadth of novel cell and gene therapy development and evaluation across a number of neurodegenerative disorders.”
‘Current Challenges in Cell Therapy for Neurodegenerative Diseases’ is available to purchase in hard cover or ebook format.
Lauren Griffiths is a Research Technician at Swansea University. Her recent research has centred around cholesterol, its function in the brain, and understanding its role in neurodegenerative diseases.
Cholesterol is an essential molecule in the body, and especially in the brain, where it is the most common lipid and is essential for cell membranes, including the myelin sheath (the fatty substance that allows nerve signals to move quickly).
The synthesis and metabolism of cholesterol are regulated by enzymatic reactions, but what happens when this process goes wrong and how does it impact brain function?
The research
That was the question I wanted to answer when beginning my PhD almost four years ago, where, as part of the team that developed a novel imaging technique that, paired with mass spectrometry, allows us to accurately map and measure cholesterol across intact brain tissue sections.
This method of mapping and measuring cholesterol in the brain was the first of its kind and has come at a really important time where interest has turned to how cholesterol, and its derivatives, play important roles in neurodegenerative diseases like Alzheimer’s, Parkinson’s, and Huntington’s.
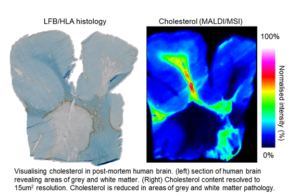
We have recently applied our method of imaging cholesterol to human multiple sclerosis (MS) tissue and collaborated with the Brain Repair Group in Cardiff University (Prof Anne Rosser and Dr Mariah Lelos) to analyse cholesterol in the brain of Huntington’s disease (HD).
What next?
The next steps in our research journey with BRAIN are to analyse the cholesterol precursors and derivatives, the oxysterols, using another novel mass spectrometry technique. Oxysterols are important signals to protect neurons from dying and reduce brain inflammation.
One important oxysterol that we are now focussing on is 24S-hydroxycholesterol, which is linked to neuronal loss and when its synthesis is boosted can prevent neurodegeneration in animal models.

Around 145,000 people live with Parkinson’s in the UK, and it’s the fastest-growing neurological condition in the world. For World Parkinson’s Day, Dr Emma Lane from the BRAIN Unit discusses the disease and some things you may not know.
What is Parkinson’s disease?
Parkinson’s disease is a neurological condition that causes progressive damage to the brain over many years. People with Parkinson’s don’t have enough of the chemical dopamine because some of the nerve cells that make it have died.
There are lots of different treatments and therapies available to help manage the condition.
It affects around one in 500 people but this increases with age, rising to one in 100 people over 60 years old and 3 in 100 people over 80. Symptoms can include tremor, slow movement and stiff and inflexible muscles.
People with the condition may also experience mental health problems such as depression and anxiety.
Facts about Parkinson’s disease
While Parkinson’s diagnoses continue to increase around the world, it’s not always the most understood condition.
1. Parkinson’s has a scent
There are some people who can actually ‘smell Parkinson’s’ and this has led to some brilliant research into how the skin may be affected by Parkinson’s and whether this can be used to detect the disease. In contrast, another symptom of Parkinson’s can be the loss of smell of certain foods like bananas, dill pickles, and liquorice.
2. Parkinson’s is more than ‘just’ a motor condition
Nonmotor symptoms are getting more attention from doctors and researchers. These symptoms include but are not limited to, cognitive impairment or dementia (usually in later stages), anxiety, depression, fatigue, and sleep problems.
For some patients, nonmotor symptoms are more disabling than motor symptoms, which are the focus of treatment.
Be sure to talk to your doctor about other issues so you can get all of your symptoms addressed.
3. Parkinson’s is not a fatal disease
Although a diagnosis of Parkinson’s is devastating, it is not, as some may still believe, a death sentence.
Parkinson’s disease is not a direct killer, like stroke or heart attack. Much depends on the quality of your care, both from your doctor and yourself. There are some very good drugs that help manage many of the symptoms.
The gait and balance changes may make you more vulnerable to falls. These are reasons why exercise and physical therapy are so important.
4. No two people have exactly the same symptoms
The progression of symptoms is often a bit different from one person to another due to the diversity of the disease and changes as the disease progresses.
Many people think of Parkinson’s as the ‘one where you shake’. In fact, only about a third of people experience tremors as part of their disease.
People with Parkinson’s may experience slowness of movements, limb rigidity, changes in the way they walk, and problems with balance.
A change in handwriting, specifically handwriting that’s become smaller or more crowded, or a less expressive face, are also symptoms.
5. The cause is unknown and there is currently no cure
What causes Parkinson’s remains largely unknown.
Genetics cause about 10 to 15 percent of all Parkinson’s. The other 85 to 90 percent of cases are classified as ‘sporadic’ or ‘occasional’.
Although there is currently no cure, which organisations like Parkinson’s UK are working to change, treatment options vary and include medications and surgery.
6. Running or walking?
People with Parkinson’s often find other forms of activity easier than walking.
Running or riding a bike can be easier than walking.
Getting through doorways can be a particular challenge and people with Parkinson’s have strategies to deal with circumstances that make them ‘freeze’ at lines on the carpet or doorways.
7. What you eat makes a difference
The drugs that treat Parkinson’s disease help replace the chemical in the brain, dopamine, that is lost as the brain cells die. This can work very effectively but it can be improved with changes in diet.
High levels of protein in the diet can stop the drugs from getting to the brain to do their job, so managing when and what you eat around your medication can make a huge difference to their effects.
8. Treating Parkinson’s
For people with Parkinson’s, exercise is more than healthy, it’s a vital component of maintaining balance, mobility, and activities of daily living.
Exercise and physical activity can improve many of its symptoms. A minimum of two and a half hours a week can slow the decline in quality of life.
Tai chi, yoga, Pilates, dance, weight training, and non-contact boxing can all have positive effects.
Your Parkinson’s specialist will be able to support the management of your symptoms with medication and guidance for other forms of support
Seeking medical advice
If you’re concerned that you or someone you know may have symptoms of Parkinson’s disease then it’s advised to see a GP.
They’ll ask you about the problems you’re experiencing and may refer you to a specialist for further tests.
Work at the BRAIN Unit
Dr Lane concludes: “10 years ago, commercial research into neurodegenerative diseases was struggling. There has been a huge shift recently with several exciting and diverse approaches to treating Parkinson’s reaching clinical trials.
“At the Brain Unit, we are passionate about ensuring our patient community voices are heard as part of these exciting developments and they are on this journey with us in the search for effective treatments.”
Learn more about work underway with BRAIN Involve, the BRAIN Unit’s public and patient involvement group made up of people who are, or have been, affected by neurological diseases.
Purple Day for Epilepsy takes place every year on March 26. To mark the global awareness day this year, Peter Roberts from BRAIN Involve has kindly shared his own story of being diagnosed with epilepsy and how he has supported neuroscience research at Cardiff University over the past two decades.
Peter’s first epileptic seizure was in the bathroom on 12th September 1994. It was followed by another seizure the next month and another in March 1995. Peter visited the hospital for a check-up and minor scan and no cause was found, but it was thought to be idiopathic epilepsy.
Peter said: “My doctor placed me on Epilim Chrono and I lost my driving licence for a year. As I worked in Aberdare and I had to travel to and from Barry, this caused a few problems, especially as commuting by train wasn’t totally reliable.
“I was taken off the tablets in 2006 but in 2007 I had another seizure and lost my licence again for a year. I have, as a precaution, stayed on Epilim ever since. To this day no cause has been found for my problem.”

Peter’s diagnosis of idiopathic epilepsy and the medication he takes to manage the condition have had an impact on his life.
He added: “Losing my driving licence has been the greatest inconvenience for me and I think Epilim has caused me recurring minor skin problems. It has also impacted my wife to a minor degree as she is always there to check I’m taking the tablets!”
After his diagnosis, Peter was asked to join the WERN group (Welsh Epilepsy Research Network): a group of people with epilepsy, led by doctors and researchers from Cardiff University, who met once a month to discuss their experiences and challenges.
Peter said: “Patients and family members were welcome at the WERN meetings which were held in Cardiff or Bridgend. One of the main doctors was Dr Cheney Drew and when this group folded, Cheney asked me if I would join BRAIN Involve. I gladly accepted and the rest is history.
“I have talked to researchers, students, and patients about likely problems and now meet people with Multiple Sclerosis, Parkinson’s Disease, and Huntington’s Disease.
“There are various levels of epilepsy, mine is minor and appears well controlled. Others are not so lucky, having multiple seizures every day and night and requiring full-time care. This is bound to have an effect on their education, job prospects, and all that follows in their future life.
“Research, like the work happening at the BRAIN Unit, is so vital for these people so that they can regain some sort of normality in everyday life. I’m really pleased to play my part in supporting the research by being a member of BRAIN Involve.”
BRAIN Involve is a public involvement group made up of people who are, or have been, directly affected by neurological diseases such as epilepsy, Huntington’s disease (HD), Multiple Sclerosis (MS) or Parkinson’s disease (PD).
By bringing their personal experiences to the research table, members contribute to the design, development, implementation, and dissemination of the BRAIN Unit’s research around brain repair and developing new therapies for brain conditions.

Peter concluded: “Sharing our lived experiences of epilepsy and other neurological diseases at BRAIN Involve can really have an impact on shaping the neuroscience research happening at Cardiff University and increase awareness of these conditions.
“If any member of the public knows of a family member or friend within any of the four problem areas listed above, please come along to our next meeting. We are currently meeting virtually and you would be very welcome. Never be afraid of asking for help, there will always be someone only too glad to be of assistance.”
BRAIN Involve brings together patients, carers, and academics to shape cutting-edge research into neurological and neurodegenerative diseases. You can find out more about how to get involved on our website.
A special thanks to Peter for sharing his story for Purple Day 2022.
In the 2018-20 award, the BRAIN Unit received funding to develop an Electronic Patient Record (EPR) system supporting clinical care and deep patient phenotyping in Multiple Sclerosis (Cardiff and Vale and Aneurin Bevan), Parkinson’s Disease (Abertawe Bro-Morgannwg) and Epilepsy (Cardiff and Vale).
The system is deployed via a secure internet-facing server behind the NHS firewall, allowing researchers to securely collaborate and contribute patient-level datasets. Towards the end of the award, a new multi-disciplinary module for the epilepsy surgery programme (Cardiff and Vale) was deployed. The PatientCare database is now well integrated and has cross-disciplinary use, improving the care of patients.
Developing the EPR system
We now wish to expand on this platform to develop research-ready cohorts, where detailed diagnostic and clinical phenotype data is maintained alongside patients’ consent to be approached for research, and tissue biologicals, most commonly serum and plasma for genetic and other disease biomarkers are collected and stored.
A programme is already in place for Multiple Sclerosis for patients in South Wales led by Professor Neil Robertson, utilising a clinical database ‘PatientCare’ and the Wales Neuroscience Tissue bank. We are developing a similar pipeline for patients with epilepsy, the PatientCare database is already being used to capture diagnostic and treatment data as part of routine clinical care.
Additional funding from the BRAIN Unit will go towards extending this work to a formal research proposal with NHS Ethics and R&D approval for tissue and para-clinical (namely brain scan (MRI) and electroencephalograph (EEG)) data collection with patient consent for storage and onward research, for patients with epilepsy attending specialist clinical in Cardiff and Vale and Cwm Taf health boards.
This supports one of the main objectives and strengths of BRAIN, which is the close bidirectional link between academic research and routine NHS clinical care, giving access to patients with neurological conditions attending outpatient clinics into clinical research and clinical trials.
Expanding the team
To execute this research, we welcomed Valerie Anderson to the BRAIN Unit team, to support an epilepsy clinical database and sample collections setup, initially working on the protocol, ethics and R&D approvals.
This will be of benefit to other researchers in epilepsy, who will have access to the data and samples collected, create research-ready cohorts for clinical trials and studies as they develop, that would be available for any BRAIN Unit investigators and outside collaborators. And it will open opportunities for collaborations with other research initiatives in the UK and internationally.
Valerie previously established a similar project in Multiple Sclerosis. Her experience and knowledge from doing this will allow us to proceed at pace in getting things set up for epilepsy, and then to work further on the running of the project once set up.
Once established, as envisaged within the 12 month funding period recruitment, consent, sample collection and data collation would continue through standard clinical encounters. Data would be available for research and follow-on funding would be sought for both infrastructure and project-specific support.
BRAIN Involve would like to help researchers consider the benefits of involving the public in forming their research into neurological and neurodegenerative conditions.
BRAIN Involve is a public involvement group made up of people who are, or have been, directly affected by neurological diseases such as epilepsy, Huntington’s disease (HD), Multiple Sclerosis (MS) or Parkinson’s disease (PD).
By bringing their personal experiences to the research table, members contribute to the design, development, implementation, and dissemination of research around brain repair and developing new therapies for brain conditions.
Complete the survey
Complete the brief survey today to help us understand to what extent PPI is used in neurological and neurodegenerative conditions and see how BRAIN Involve could shape and inform your research.
Jack Fisher a Cardiff University Student Doctor currently working with BRAIN researcher Dr Malik Zaben won the award for best oral presentation at this year’s CITER Annual Scientific Meeting.
The Cardiff Institute for Tissue Engineering and Repair Annual Scientific Meeting (CITER ASM) took place virtually this year. This event is an opportunity for academics, early career researchers, MSc students, PhD students and undergraduates to discuss the latest research findings in the research areas of Stem Cell Science, Tissue Engineering and Repair and Disease Translation.
Jack Fisher’s project examined the effects of injury condition medium on the expression of the transcription factors Pax6 & TBr2- key regulators of cortical neurogenesis.
Fisher is the second BRAIN Unit researcher to be awarded first place for his oral presentation as Dr Ronak Ved proudly took home the prize in 2020.
Dr Ronak Ved has been awarded a Medical Research Council (MRC) Clinical Research Training Fellowship in the field of traumatic brain injury.
The prestigious scheme provides predoctoral researchers with the opportunity to foster a competitive PhD research, moving towards a career as a clinical scientist.
Ronak explained: “As a neurosurgical registrar at the University Hospital of Wales, I regularly witness the devastating effects traumatic brain injury (TBI) can have upon patients and their families.
“Thousands of patients suffer a head injury every year, and this costs the NHS billions of pounds in resources. This has inspired me to want to investigate how neurotrauma affects brain tissue, and to try to identify ways in which we may be able to protect or repair brain cells in patients who have had a head injury.”
There are few therapeutic agents which have been shown to protect brain cells after head injuries.
“This might partly be because most studies in this field have a) focussed on using animal models of TBI, and b) only rarely reviewed how neurotrauma damages connections between brain cells, known as white matter.
“My project will focus on using human tissue samples, kindly donated by patients of the neurosurgical department at the University Hospital of Wales, to assess how trauma influences the cells that make up the white matter of the human brain. We’ll also be able to use these human cell samples to search for drugs which might protect or repair human white matter in people who have had a head injury.”

Ronak will be working under the supervision of Dr Malik Zaben and Professor Liam Gray, in the Brain Research And Intracranial Neurotherapeutics (BRAIN) Unit of Cardiff University.
“The opportunity to work with human brain tissue is a rare privilege, and I am very much looking forward to working on this exciting project. We hope to use it as a springboard for further work which would support our clinical practise as neurosurgeons in the future, to help improve outcomes for patients who have suffered a TBI.”
Get involved
Interested in sharing your experience to shape research? Or are you a researcher looking to include the public in your work?
We’d love to hear from you. Complete our short form to register your interest.
A researcher from the BRAIN Unit and Neuroscience and Mental Health Research Institute (NMHRI) at Cardiff University has been awarded the Guarantors of the Brain Fellowship.
Dr. Malik Zaben works across the Division of Psychological Medicine and Clinical Neurosciences at Cardiff University. He is a lecturer in neurosurgery with a special interest in understanding neurogenesis and neuroplasticity after traumatic brain injury (TBI). His research explores potential therapeutic approaches targeting neuroinflammatory pathways to limit brain damage after injury, and enhance repair.
The Guarantors of Brain is a charity that aims to promote teaching, education, and research in neurology and related clinical-academic disciplines and Dr. Zaben is a recipient of their Brain Clinical Post Doctorial Fellowship for 2021.
Dr. Zaben said “I am delighted to receive the Guarantors of Brain Fellowship award.
“Traumatic brain injury (TBI) causes significant mortality and morbidity globally, with many survivors suffering longstanding neurocognitive, motor, and sensory deficits that profoundly impair their ability to function independently.
“Understanding how neuroinflammation influences cortical neuronal regeneration after TBI is essential to facilitate the identification of novel therapeutic strategies to improve TBI-associated neurological deficits.”
Researchers from the BRAIN Unit and NMHRI have previously undertaken pre-clinical observations in animal models which highlighted positive steps forward in the development of pharmacological strategies to enhance brain repair after injury. However, key neuroinflammatory processes after injury remain poorly understood, particularly in the human brain.
Dr. Zaben added: “Although animal models have been useful in understanding many processes in TBI, the extent to which TBI animal models replicate the human brain’s response to injury has been questioned rendering them less useful for exploring pharmacological approaches.
“The new fellowship award will facilitate focused research on the use of adult human cortical cells.
“The important damage-associated molecule, High-Mobility Group Box 1 (HMGB1), impacts stem cells’ fate. HMGB1 works via toll receptor subtype 4 (TLR4) and the receptor for advanced glycation end-products (RAGE) to initiate neuroinflammation in many brain pathologies. I will examine the HMGB1-TLR4-RAGE pathway in human cortical inflammation and neuronal regeneration after injury, examining internal nervous system stem cell capacity to repair the injured human brain.
I’d like to thank the Guarantors of the Brain for this fellowship and look forward to undertaking further lab-based research over the next year, made possible by this award.”
Read more about Malik’s ongoing research into traumatic brain injury here.